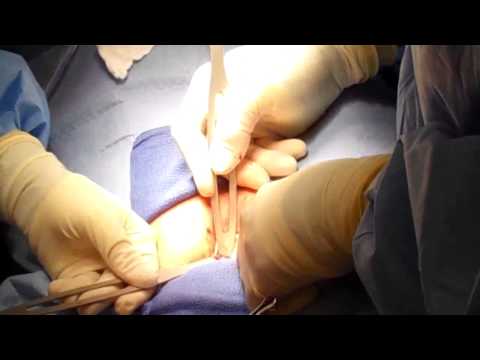
What is Essure?
Essure is the only permanent birth control for women that does not require a skin incision. The Essure is similar to the traditional IUD in that the implantation procedure does not require anesthesia nor does the device contain or release hormones into the patient. Essure implantation is an in-office procedure and more cost effective than tubal ligation.
The Essure device consists of three components:
- An inner plastic fiber
- A flexible stainless steel inner coil.
- An outer nickel titanium alloy coil.
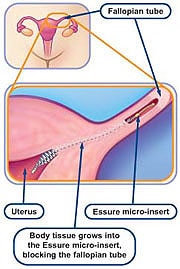
The procedure consists of implanting one of the spiral coils in each of the fallopian tubes. Over a 3 month period, tissue forms around the coils creating a barrier. That barrier prevents sperm from reaching the egg which prevents conception.
Since the FDA approved Essure in 2002, the success rate of preventing pregnancies rests at 99.83%. However, some women have complained of severe complications from Essure.
Essure Complications
The FDA states that some women have experienced painful health complications after Essure implantation. One of the side-affects, noted on the Essure labeling, is pain. But in a study, conducted by the FDA from 2002 to 2013, women also noted experiencing hemorrhage, headaches, menstrual irregularities, extreme fatigue, depression, and weight gain. Other cases noted a device malfunction, either breakage or the device was not positioned properly. The FDA also suggested that because the outer coil is made from nickel-titanium, some women may have a (nickel) allergy to the device.
The agency acknowledges there is evidence of complications from Essure, but it still considers the device a safe option for permanent birth control. However, if you are experiencing pain or other complications, it is important that you are evaluated by your doctor for the cause of discomfort. If that discomfort is due to your Essure device, there is no medical team more experienced than NCCRM.
UPDATE: 9/23/15 – Federal medical experts will take a closer look at a host of problems reported with the birth control implant called Essure, including chronic pain, bleeding, headaches and allergic reactions.
The Food and Drug Administration on Monday posted a 90-page review of Essure online, ahead of a Thursday meeting where experts will re-examine the safety and effectiveness of the implant.
Read full article here.
Essure Vs. Adiana
Both the Essure and Adiana Occlusions are similar and require the same procedure to reverse them. The Essure device has only been available in the last decade, but we are now starting to see a higher number of requests to have this type of tubal occlusion reversed. We have successful pregnancies resulting from Essure and Adiana and we can help you too.
The Essure and Adiana devices are supposed to be permanent and not reversal, similar to traditional tubal ligation, but at the North Carolina Center for Reproductive Medicine (NCCRM), we have the expertise in advanced micro-surgery to perform this procedure.
The procedure to reverse an Essure or Adiana is different than a standard tubal reversal. What is required is called a tubocornual implantation. The old way to do a tubocornual implantation was very hard to do and left the patient requiring a cesarean section for future pregnancies. With the way we perform this procedure at our facility this is no longer the case.
To do this type of reversal, the Essure or Adiana device needs to be first carefully removed. The next step is to make a tiny, perfectly round hole in the wall of the uterus. Once the uterus is prepared, the tube is sewn deep into the lining of the womb. The tube is next sewn to the outside of the uterus to seal it off.
If you are experiencing negative side effects from your Essure and want to have it removed, not reversed, please read more here.
Please call our office and speak with one of our clinical staff to answer any questions you may have.
Surgery Process:
Adiana Reversal Surgery is similar to a tubal ligation reversal procedure requiring skilled surgeons. In this situation, a new opening can be created through the uterine muscle and the remaining tubal segment inserted into the uterine cavity. This microsurgical procedure is called tubouterine implantation, uterotubal implantation, or, simply, tubal implantation. Tubal implantation is performed when tubal anastomosis is not possible due to the absence of a proximal tubal segment and interstitial tubal lumen.
Click here for discharge instructions after Adiana, Essure and Tubal reversal surgery.
Dr. Sameh Toma founded NCCRM in the 1990’s and was one of the first private fertility centers in North Carolina. Other UNC fertility doctors joined Dr. Toma and NCCRM in providing Tubal Reversal, IVF, and other fertility services in a more efficient and affordable private setting.
Dr Toma is the medical director and does the majority of our surgeries. He is one of the most experienced fertility doctors in the world, specializing in Tubal Reversal Surgery and In Vitro Fertilization. Dr. Toma was trained in microsurgical tubal reversal surgery while at UNC by Dr. Hulka, a pioneer in tubal reversal surgery who developed the Hulka clip as a method of tubal ligation resulting in minimal destruction to the tubes.
At NCCRM we are proud to offer IVF and Tubal Reversal to our patients, individualizing the treatment to the appropriate patient. Patients with an ample amount of tube may do best with tubal reversal while those with minimal tubal length may do best with IVF. IVF is also best when there is a male factor. That is why we recommend a semen analysis prior to a tubal reversal.
NCCRM provides the best success at one of the best prices in the industry by providing high quality service in a most efficient process. An example is how we do liposuction to decrease the abdominal thickness in patients with a higher BMI. This allows better access to the tubes. The result is a better-quality anastomosis that results in a higher chance of a successful pregnancy. NCCRM is the only fertility practice with liposuction capability and it still less expensive than most infertility clinics charge for a tubal reversal alone. This is one of the advantages that helps make our success rates the highest on the East Coast.
NCCRM was first in the world to do both Essure and Adiana reversals. Our years of experience has allowed us to continuously yield the highest success rates in the world for these procedures. Please follow us on Facebook to see all the success stories from our wonderful patients and we look forward to adding your story as you become a part of the NCCRM family.
Fee for Essure and Adiana surgery: $7,300+
After discount($8,400 – $1,100)
A Safe Solution: Essure Removal at NCCRM
The North Carolina Center for Reproductive medicine (NCCRM) is proud to offer a safe solution for women who are suffering from Essure complications. We have heard countless stories from women who are dealing with Essure side effects, ranging from severe headaches and abdominal pain to colon perforation. Our experienced medical team can relieve your discomfort with a safe Essure Removal.
Dr. Sameh Toma is a microsurgeon who is highly experienced in safely removing the Essure device. While the Essure insertion is done vaginally and without anesthesia, microsurgery is required to remove it. When the Essure device is inserted into the fallopian tube, a barrier wall of tissue is formed to block sperm from reaching the egg. Within 3 months the device is embedded into the walls of the fallopian tubes. This microsurgery is done in order to safely remove all three components of the device and any coil fragments.
For women who still do not want to become pregnant, a tubal occlusion is done at the time the Essure device is removed. The microsurgery takes about one hour and is done under general anesthesia through a 2-4 inch bikini incision. Recovery is usually five to seven days.
Women who visit NCCRM know they are in good hands with the experienced, micro-surgical skills and techniques of Dr. Toma for a safe Essure removal and tubal occlusion.
Fee for Essure Removal:
Fee: $5000 + $300 Consult/Ultrasound (Please call 919-233-1680 ext. 180 for more information.)
If you are wanting to restore your fertility after removing the Essure coils, the fee is $7000 + $300 Consult/Ultrasound. The $7000 fee is only for the removal of the Essure coils. ** Please note, the upper limit BMI to qualify for surgery at any out patient surgery center is 35. You can find out your BMI here.
For some women, they carry excess weight around their bikini area that makes it difficult for the surgeons to access the area they need to operate. In that case, our surgeons may perform liposuction on that bikini area immediately before the Essure removal surgery. If liposuction is deemed necessary, there will be an additional $1000 additional fee in order to accomplish the Essure removal.
FAQ’s
If I have the Essure Device removed will my symptoms go away?
While there is no guarantee that your symptoms will improve or completely dissipate, it appears that Essure removal will help the majority of women who are having Essure Device related problems.
If I have the Essure Device removed will I get pregnant?
Removal of the Essure Device will not restore your fertility since your fallopian tubes will not be attached to your uterus.
Why is it important that a microsurgeon remove the Essure Device?
Because of the method in which the Essure Device was constructed, each of its three components can be fractured (and left behind) if not meticulously performed by a microsurgeon, like Dr. Sameh Toma. Leaving behind a piece of the Essure Device may not allow improvement of symptoms.
My physician recommends that I have a hysterectomy to remove the Essure Device and improve my symptoms.
A hysterectomy may be the appropriate surgical approach, especially if there is other pathology such as fibroid tumors, polyps or ovarian cysts. However, a hysterectomy is a much more extensive surgery associated with more complications than microsurgical removal of the Essure Device. You must decide, after weighing the pros and cons of these options, what is the optimal procedure for you. Not all physicians can remove an essure device, so they might recommend hysterectomy.
I have no adverse symptoms from my Essure procedure but I am planning to undergo IVF (in vitro fertilization) in the next few months. Should the Essure Device be removed?
Yes it should be removed prior to undergoing IVF.
If you are interested in moving forward with Essure removal, please fill out these forms and submit them safely through our website. Our staff will be in touch with you after you have sent us the completed forms.
To learn more or schedule a consultation:
Call (919) 233-1680 or